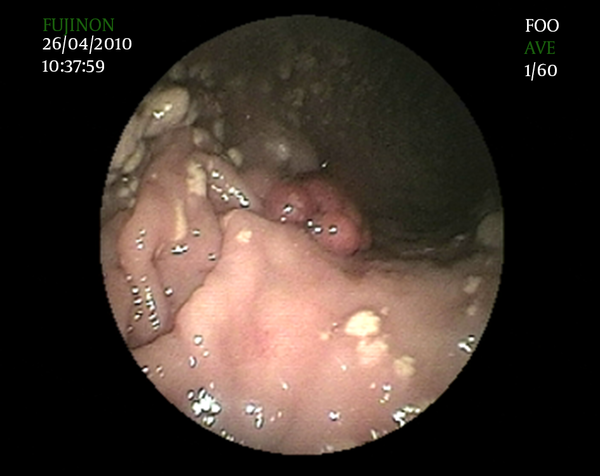
Xanthelasmas are a particular type of Xanthoma. Xanthomas can appear on any part of the human body and are addressed as Xanthelasmas whenever they appear on the eyelids or around the eyelids.
What is Xanthoma?
Xanthoma are fatty growths underneath the skin. These growths can appear anywhere on the body. Basically it is a fatty growth that starts accumulating below the skin and ultimately protrudes from the surface of the skin. Xanthoma are fatty patches inside the skin.
Xanthomas can vary in size. These growths may be as small as a pinhead or as large as a grape. They often look like a flat bump under the skin and sometimes appear in yellow or orange color. These are usually not painful, however, they might be tender and itchy. They can grow in clusters in the same area or several individual growths on different parts of the body.
Where they can Appear?
These growths can appear anywhere on the body, but they typically form on the:
- Joints, especially the knees and elbows
- Hands
- Buttocks
- Feet
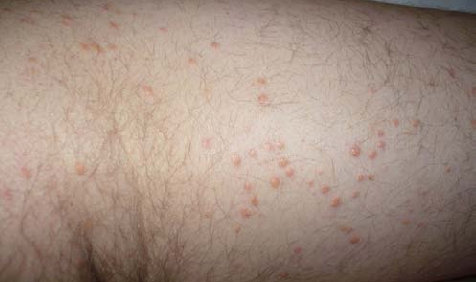
Xanthoma may appear as single lesions or as a cluster. It may develop on one part of the body, or can affect different parts. These lesions can appear in different shapes and sizes. Some people may have a xanthoma which is as large as grapes, whereas others can have xanthomas as small as a pinhead. Usually, these lesions appear as small bumps inside the skin which may be yellow or orange color. These lesions can be itchy and may be slightly tender to the touch at times, however, mostly they are not painful at all.
What Causes Xanthoma?
Xanthoma is usually caused by high levels of blood lipids, or fats. This maybe a symptom of an underlying medical condition, such as:
- hyperlipidemia, or high blood cholesterol levels
- diabetes, a group of diseases that causes high blood sugar levels
- hypothyroidism, a condition in which the thyroid doesn’t produce hormones
- primary biliary cirrhosis, a disease in which the bile ducts in the liver are slowly destroyed
- cholestasis, a condition in which the flow of bile from the liver slows or stops
- nephrotic syndrome, a disorder that damages the blood vessels in the kidneys
- hematologic disease, such as monoclonal gammopathy metabolic lipid disorders. These are genetic conditions that affect the body’s ability to break down substances and to maintain important bodily functions, such as digestion of fats.
- cancer, a serious condition in which malignant cells grow at a rapid in uncontrolled rate
- side effect of certain medications, such as tamoxifen, prednisone, and cyclosporine
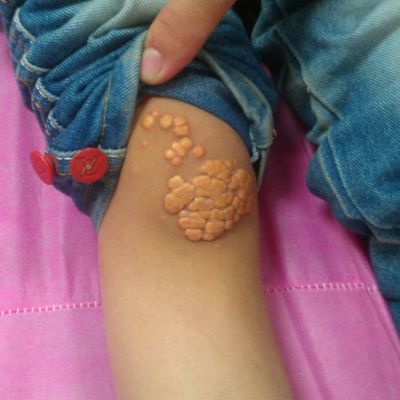
Types of Xanthoma
There are many kinds of xanthoma. Some are differentiated based on their color or contents, others are differentiated based on their causes and there are some others which are differentiated based on their shape.
Xanthomas are like tumors—a collection of foamy histiocytes in the dermis. They may be associated with familial or acquired disorders resulting in hyperlipidemia with no underlying medical disorder. Tuberous xanthoma form as yellow nodules and are frequently associated with hypertriglyceridemia, but they are also seen in patients with hypercholesterolemia.
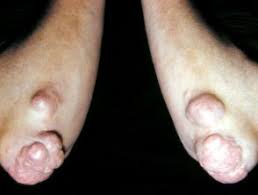
We have presented a case of multiple tuberous xanthoma in a subject with normal lipid metabolism and with no associated systemic disorders, which is an uncommon occurrence. This case is being reported because of its rare occurrence. The aim of this report is to emphasize that the patient has a normal lipid profile.
Causes of Tuberous Xanthoma
All xanthoma are primarily caused by elevated levels of fat in the blood and body. This leads to excessive deposition of fat in tissues, the production of foamy cells and eventually xanthoma. Here, some factors are responsible for the predisposition of developing Xanthoma.
Obesity, elevated levels of lipids and cholesterol in the blood are responsible for this condition that results in the availability of fats for consumption by macrophages. Hyper-cholesterolemia, the elevated cholesterol in the blood, which leads to deposition of cholesterol crystals in the body which is consumed by macrophages and clustered as foamy cells and ultimately, xanthoma.
Genetic diseases and familial conditions may lead to elevated levels of lipid in the blood and hence predispose to the development of tuberous xanthoma.
- Firm, uncomplicated, red-yellow nodules that develop on the stressed areas like— knees, elbows, and buttocks. These are a little different than the typical xanthelasma definition but follow the same pattern.
- Lesions can be accumulated together to create multi-lobulated masses
- Usually associated with hypercholesterolemia (increased cholesterol levels in blood vessels) and increased LDL levels.
- These xanthomas are firm swellings that lie deep in the subcutaneous layer of the skin.
Symptoms of tuberous xanthoma
- Gross deformity, the lesions can look unsightly and are a cosmetic disfigurement, in such cases patients usually seek help.
- Painless, the lesions of tuberous xanthoma are not painful and usually resolve after lipid abnormalities are corrected.
- Hyper-pigmentation, the tuberous xanthoma or plaque can lead to increased pigmentation, which causes cosmetic disfigurement.
Xanthoma are commonly caused by exess lipids in the body which are not metabolised correctly. Tendonous xanthoma are cholesterol deposits in tendons. They appear as enlarging papules or subcutaneous nodules attached to tendons, ligaments, fascia, and commonly affect the tendons of the dorsal surface of the hands and the Achilles tendon. Their presence is a possible clinical sign of familial hypercholesterolemia, high LDL cholesterol levels, and premature cardiovascular disease.
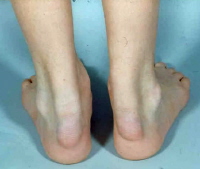
As mentioned earlier they appear as subcutaneous nodules attached to tendons or ligaments
- The yellow plaques as stated in the xanthelasma definition occur most commonly in the hands, feet, and Calf muscles.
- They are primarily attached to tendons and are commonly found at the Achilles tendon at the ankle and the extension tendons of the fingers.
Causes Tendinous Xanthoma?
- Familial hyper-cholesterolemia, there is a deficiency of LDL receptors that result in the accumulation of cholesterol-laden byproducts of VLDL.
- Obesity, an overall increased level of fat in the body that leads to the accumulation of cholesterol and triacylglycerol in body tissues and the production of fat cells.
- Hypothyroidism, diminishes the utilization of fat by decreasing the core metabolic rate of the body, causing elevated levels of resources in the blood.
- Diabetes, the excessive amount of sugar is converted to fat and stored in tissues where it triggers macrophages to consume it and transform into foam cells.
They maybe correlated with hypercholesterolemia and enhanced LDL levels.
Plane Xanthomas are the flat type of xanthomas which can appear anywhere on the body. However, depending on where they grow on the body these type of lesions grow due to certain particular causes. So depending on the location of these types of Plane plaques, the possible underlying causes can be sometimes identified but not always.
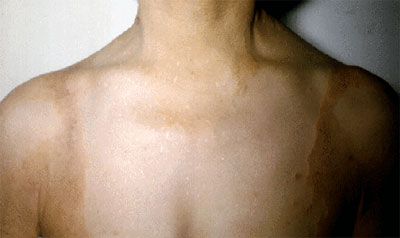
Diffuse Plane Xanthomas
Diffuse Plane Xanthomas
Diffuse plane xanthoma (DNPX) was first described by Altman and Winkelmann in 1962. It is an uncommon subtype of xanthoma characterized by diffuse plane xanthoma of the head, neck, trunk, arms, and legs; They can develop while having normal cholesterol levels. This type of Xanthoma typically appear first on the neck and upper trunk.
These lesions are due to a rare type of macrophage disfuction. The defect results in the presence of an abnormal antibody in the blood called a paraprotein. This kind of Xanthoma can be correlated with certain types of cancers meaning that people with Diffuse plane Xanthpomas can have a higher likelihood of developing cancer. This type of xanthoma can also develop on the neck, face, chest, buttocks, armpits, and groin.
.
- Presents with large level reddish-yellow plaques over the facial skin, neck, breasts, and buttocks and in skin folds (like the armpits and groin).
- An exceptional form of histiocytosis that is different from the typical xanthelasma definition.
- Caused due to an unusual antibody in the bloodstream called a paraprotein.
- Lipid levels are normal.
- About 50% will have a malignancy of the blood vessels; usually multiple myeloma or leukemia.
There are a number of different versions of the same disease, some more aggressive than the last. Plane Xanthoma and diffuse planar Xanthoma, are skin lesions caused due to elevated lipids in the body. Plane xanthoma is one kind of skin disorder that commonly occurs among people with high levels of blood cholesterol or triglycerides. Here we describe the exact features of this skin disorder, along with the causes and symptoms to give you a broad view of the disease.
Causes of Plane Xanthomas
- Hypertriglyceridemia, again this is due to obesity, diabetes, hypertension which can compound a number of problems.
- Hyperlipoproteinemias, a certain genetic diseases can result in impaired degradation or excessive production of lipids, which cause high levels in the blood.
- Hypercholesterolemia, due toin a malformed LDL receptor leading to high levels of LDL. This lipoprotein contains cholesterol, which can accumulate in tissues and lead to plane xanthoma.
Eruptive Xanthomas are small red to yellow papules, appearing on large clusters over the buttocks, shoulders, arms, legs or even the whole body. In certain cases, these xanthomas may appear in the mouth as well.
These xanthoma are usually tender and can be itchy and sometimes disappear over a few weeks. These xanthoma can be correlated with hyper-triglyceridemia and also with diabetes.
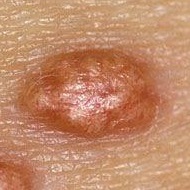
These xanthomas are usually tender and can itch and usually disappear over a few weeks. These xanthomas are caused due to hyper-triglyceridemia and are usually related to diabetes. They can present in a nodular format.
These xanthomas are miniature, yellowish papules that occur in large numbers in the same place. They are primarily found on the buttocks, but can also be found on the shoulders, legs, and arms. Their characteristic feature is that they occur in small crops and are caused due to the deposition of lipids in skin tissues. Sometimes these papules can also occur in the mouth and present as an ulcer. Another common feature of eruptive xanthomas that sets it apart is its ability to cause an itch. The lesions are also tender, which makes it important to be differentiated from the usual rash and infections.
High cholesterol may be caused by some health conditions. In turn, high cholesterol can trigger several serious diseases. Treating EX means getting rid of the excess fat in your body and treating the cause.
- Lesions typically erupt in groups of small, red-yellow papules
- Most commonly come up on the buttocks, shoulders, legs, and arms but might occur all around the body
- Rarely the facial skin and the mouth area may be affected
- Lesions may be sensitive and usually itchy
- Strong link with hypertriglyceridemia (increased triglyceride levels in bloodstream) often in patients with diabetes mellitus.
Causes eruptive xanthomas?
- Familial hyper-cholesterolemia type 2a, the disease is caused due to a genetic abnormality in LDL receptor that results in elevated levels of this fat in the body.
- Broad beta hyper-lipoproteinemia, caused due to a protein mutation that causes levated levels of triglycerides and cholesterol, exaggerating the condition.
- Hyper-triglyceridemia, which commonly occurs in hypertension, obesity, and diabetes. The elevated levels of fat in the blood leads to the formation of xanthomas.
- Diabetes, the excessive sugar is converted into fats and the tissues are surrounded by an inflammatory reaction that is difficult to control, leading to eruptive xanthomas.
More about Xathomas
Xanthoma can appear on any part of the body. They are very common to be growing on the Achilles heels. When Xanthoma appear on the Achilles heels, they found pressing on the tendons underneath the skin. The main peculiarity of this type of Xanthoma is that it grows underneath the dermis, whereas most Xanthoma are found between the dermis and epidermis.
When found on the Achilles heels, the Xanthomas can cause particular discomfort to the patient. The patient may request to have them removed because they represent an impediment comfort while walking and running. However no Xanthoma has a malignant growth and therefore, can be left untreated without compromising the longevity of the patient.

Xanthomas on Achilles Heels
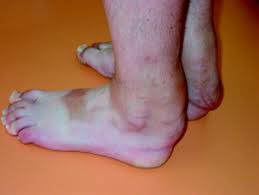
Xanthomas compromising walking and wearing standard footwear.
Xanthomas on the Achilles Heels can keep growing if left untreated. The only treatment is known to date (apart of dietary and lifestyle chages) is surgery. Surgery, for this type of condition, is only advisable once the condition becomes too discomforting to the patient. This is because, despite the simple procedure required for this type of Xanthoma removal, any surgery presents risks. Achilles heels Xanthoma surgery is particularly safe to perform because:
- No general anaesthetic is required unless the Xanthoma is particularly large.
- The area affected by the Xanthomas is not close to any important artery.
MRI and Surgery
As we can see from the Right picture, the footwear worn by the patient over time can affect the way the Xanthomas develops. Surgery for removal of this type of Xanthoma will lead to scarring. This is because of where the Xanthomas grows on the Achilles Heels inside the skin beneath the dermis itself and therefore the scar left will be due to the deep incision required for this Xanthoma removal.
This Xanthoma MRI Shows clearly how this type of Xanthoma develops inside the skin and presses on the tendons (figure A and B). Figure C at the bottoms shows how this type of xanthoma looks under the microscope. Quite similar to other types of Xanthomas and Xanthelasmas.
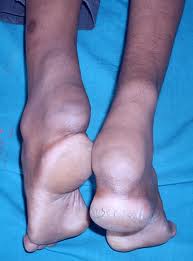
Xanthomas on Achilles Heels (Figure A)
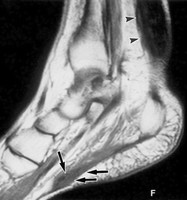
Xanthomas MRI (Figure B)
From other patient’s MRI, we can see the Achilles Heel Xanthoma pressing on the tendon as on the previous case. However, there is another Xanthomas growth underneath the Plantar Heel.
Given that after surgery the patient will not be capable of walking until they complete healing Xanthoma underneath the Plantar. Heel should only be removed if this Xanthoma becomes particularly bothersome to the patient.
The right picture shows a large Xanthoma removal. The surgeon might decide to perform this procedure under general anesthetic for large Xanthomas Removal. This procedure will inevitably leave scarring to the patient. However, the benefits of the surgery far outweighed the small risks in this case.
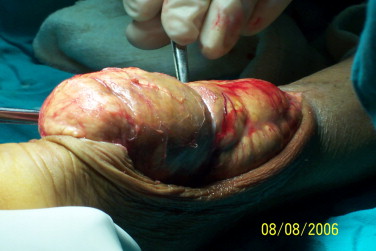
Achilles Heel Xanthoma removal
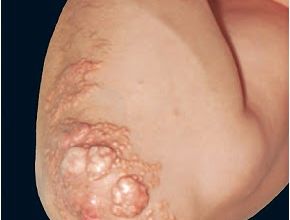
Xanthoma on the elbow
Xanthoma can develop in any part of the body. they have different characteristics depending on the area where it is developed. While the Xanthoma on the Achilles tendons grow underneath the dermis fortunately when finding them on other parts of the body they develop between the dermis and the epidermis. This, therefore, allows possible Xanthoma removal without leaving any scar.
As we can see in this particular case the patient affected is of athletic type and does not have high cholesterol levels due to his physically active lifestyle. The Xanthoma have appeared despite of his healthy lifestyle.
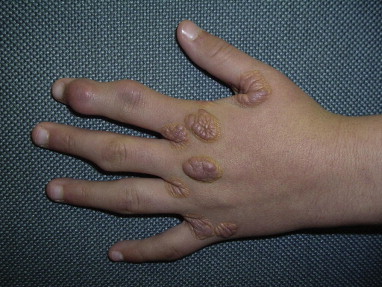
Xanthomas on Hands
Xanthoma can also appear on the back of the hands . Removal of this type of Xanthoma is possible with lasers, Hyfrecator, and other similar equipment by superficial ablation. The operator can assess the risks of scarring depending on whether the Xanthoma has affected the dermis. As stated earlier with the exception of plantar Xanthoma (including Achilles Heels Xanthoma), Xanthoma develop superficially between the dermis and epidermis.
Normally an experienced dermatologist can assess that risk of scarring by glancing at the lesion. The rule of thumb to follow in order to assess the risks of scarring, after Xanthoma removal procedures, is that the more superficial the lesion the less the risks of scarring. In case it is not possible to see the corrugation on the lesion, this means that the lesion could have grown deep into the skin and maybe underneath the dermis, but fortunately this is very rare. Therefore a deep incision is rarely required to access and remove the Xanthoma and simple superficial ablation will often suffice.
This case is not only a further demonstration that Xanthoma can appear anywhere on the body but also can be developed by individuals that are neither overweight nor have high cholesterol levels. The Xanthoma removal of this type is normally successful by simply using superficial ablation. However give the extent of the area to be treated it may require a number of sessions to achieve complete removal.
By all means it is possible to remove all Xanthoma from such a large area in a single session. The main drawback is the relatively large extent of burns that the patient is subjected to within the one session. Such a large amount of burns could pose the body to needless stress which should be avoided.
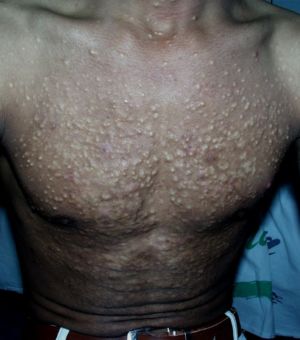
Xanthomas on Chest and Abdomen
This further example shows how Xanthoma can develop also at a young age. The removal of this type of Xanthoma is also sometimes possible by using superficial ablation as well as specialised peels.
Fortunately these types of cases are quite rare. This young patient presented overgrown Xanthoma on the Buttocks. The best proposed removal solution would be conventional surgery under general anaesthetic. However an MRI would be advisable before scheduling surgery. The MRI will provide important information concerning these benign growth inside the patient’s body.
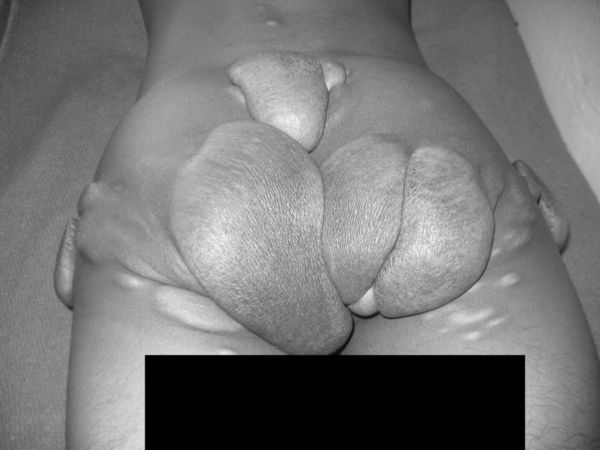
Overgrown Xanthomas
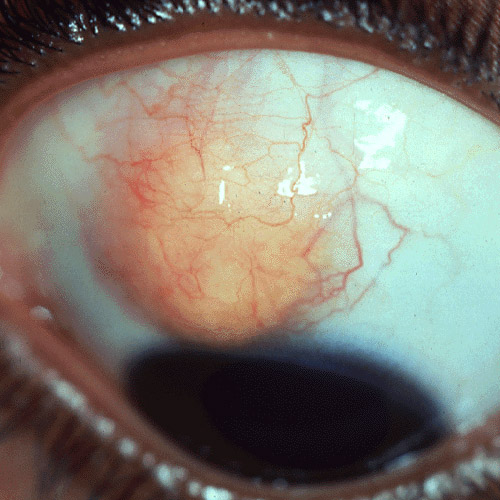
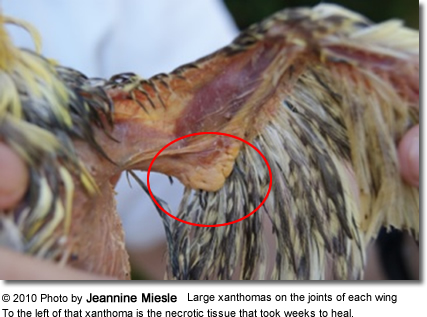
Xanthoma on eye
We thank Jeannine for this kind photo. This clearly demonstrates that Xanthoma are not a condition exclusive to us humans. Therefore if you ever develop or you have Xanthoma you know know that there little to worry. Many people have it and you may not know about it.
How Is Xanthoma Diagnosed?
Your doctor or dermatologist can typically diagnose xanthoma. They may be able to make a diagnosis simply by examining your skin. A skin biopsy can confirm the presence of a fatty deposit beneath the skin. During this procedure, your doctor will remove a small sample of tissue from the growth and send it to a laboratory for analysis. Your doctor will follow up with you to discuss the results. They may also order blood tests to check blood lipid levels, assess liver function, and rule out diabetes.
How Is Xanthoma Treated?
If xanthoma is a symptom of a medical condition, then the underlying cause must be treated. This will get rid of the growths and minimize the likelihood that they will return. Diabetes and cholesterol levels that are well controlled are less likely to cause xanthoma.
Other treatments for xanthoma include surgical removal, laser surgery, or chemical treatment with trichloroacetic acid. Xanthoma growths can return after treatment, however, so these methods don’t necessarily cure the condition. Talk to your doctor to see which treatment is right for you. They can help determine whether the condition can be treated through medical management of the underlying issue.